Melanoma accounts for about 1% of diagnosed skin cancers. Melanoma skin cancer typically starts in skin cells called melanocytes.
Diagnostic Tips
- Malignant melanoma (MM) may be a new lesion or develop in a pre-existing mole. It is twice as likely for a MM to develop as a new lesion than develop in an existing mole.
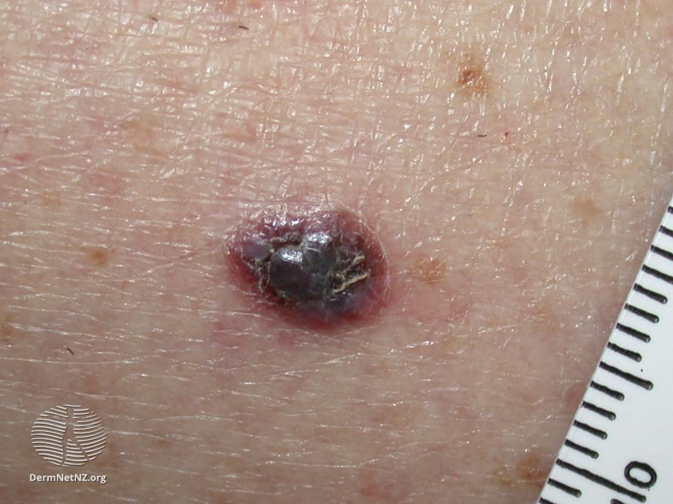
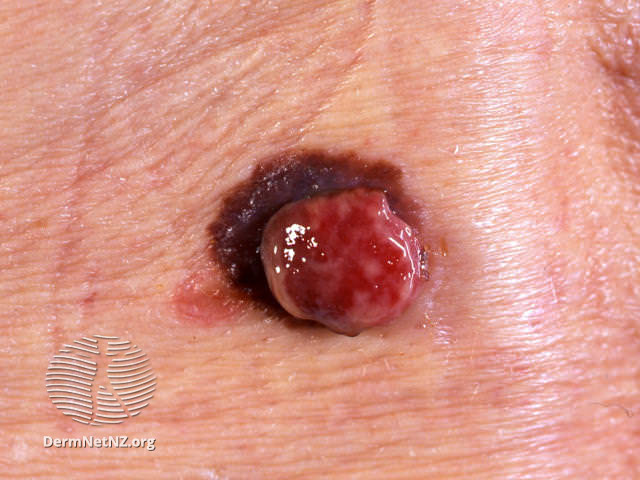
- Amelanotic malignant melanoma may present as an enlarging, granulating or smooth pink nodule. Beware the solitary pink papule!
- Skin cancers are very infrequent in those under 15 years of age
Assess risk factors:
- high sun exposure
- sun bed use
- family history of melanoma
- fair skin and a susceptibility to sunburn
- large number of melanocytic naevi (greater than 100 naevi has been shown to increase the relative risk of developing melanoma approximately sevenfold compared with 15 or less naevi)
Suspect Melanoma if there is:
The “ugly duckling” mole that doesn’t look like its neighbours!
A new mole developing in a person aged 40 or over
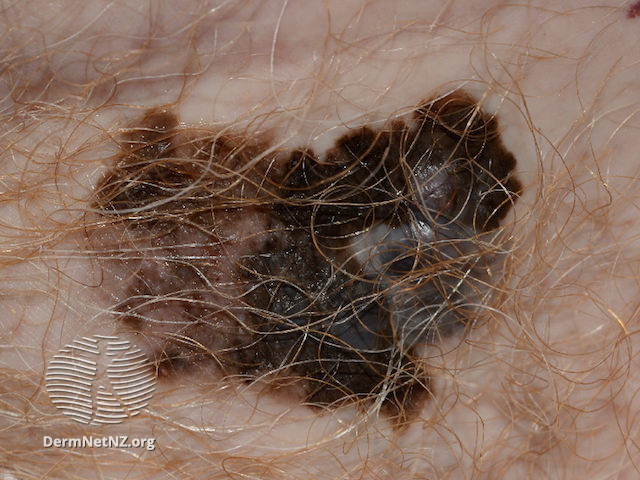
A mole with any of the following features (ABCDE criteria):
- Asymmetry
- Border (irregular, scalloped)
- Colour (irregularity or darkening)Diameter (larger lesions)
- Evolution in shape, size or colour over a quick timeframe (few weeks)
Suspect Subungual Melanoma if there is:
Nail pigmentation which evolves but remains in contact with and/or involves the nail fold (fold of skin that borders the bottom and sides of nail)
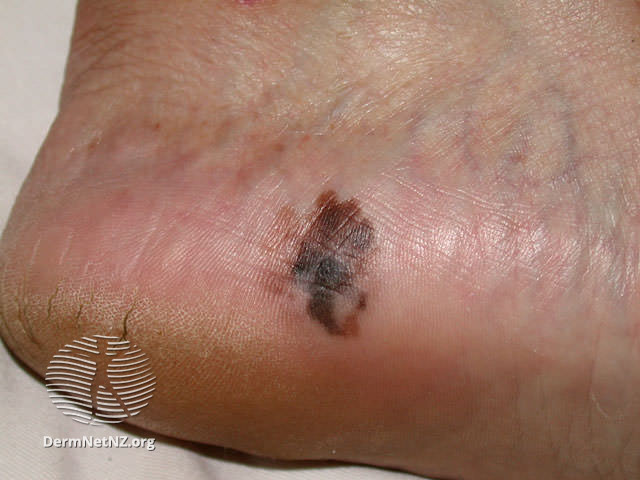
Acral-lentiginous melanoma Skin cancer can affect people of all skin colours, including those with brown and black skin. Skin cancer on darker skin often occurs on areas that get little sun exposure, like the palms of hands, soles of feet, and under/around the nails. People of colour have a higher risk of a late diagnosis and poorer prognosis as skin cancer may be less noticeable or less expected in their skin.
All images on this page are sourced from DermNet | Dermatology Resource (dermnetnz.org)
Other skin lesions that are concerning for malignancy
The following skin changes should raise concern for a malignant lesion (including Merkel’s tumour, sarcoma, or amelanotic melanoma):
- Nodule grows quickly (over weeks)
- A new change (growth, pigmentation, or pain) in a long-standing ulcer, scar, traumatic or inflamed area of skin
- Non-healing and/or destructive atypical ulcer
- Progressive unexplained scar-like area
- An unexplained skin lesion with loco-regional lymphadenopathy
Please refer these via the Melanoma pathway below.
B.C, C.L & P.O – 16-03-2026
Refer as USOC via Sci Gateway: Lauriston/SJH>Dermatology>LI Suspected Melanoma.
Please use the Using the Consultant Connect App – RefHelp to take photos of the lesion(s) and then attach these to your Sci Gateway referral.
Attaching photos to referrals – RefHelp
Any patient who has a malignant melanoma removed in primary care must be referred USOC via the above pathway.
For Patients
The BAD (British Association of Dermatologists) have several PILs on melanoma depending on the stage of the disease. These can be found at: https://www.skinhealthinfo.org.uk/a-z-conditions-treatments/ & search for “melanoma”.
For Healthcare Professionals
Primary Care Dermatology Society – http://www.pcds.org.uk/clinical-guidance/melanoma-an-overview1
Scottish Referral Guidelines for suspected Cancer – Scottish Referral Guidelines for Suspected Cancer 2025
Dermnet nz – https://www.dermnetnz.org/topics/melanoma/